Folliculitis After Waxing: Causes, Prevention, and Safe Treatment
- Understanding Folliculitis After Waxing
- Why Folliculitis Happens After Waxing
- How To Prevent Folliculitis Before, During, And After Waxing
- Safe At-Home Treatment For Folliculitis After Waxing
- Special Considerations For Different Areas And Skin Types
- When To See A Doctor And Medical Treatment Options
- Take Control Of Post-Wax Skin Health
- Frequently Asked Questions
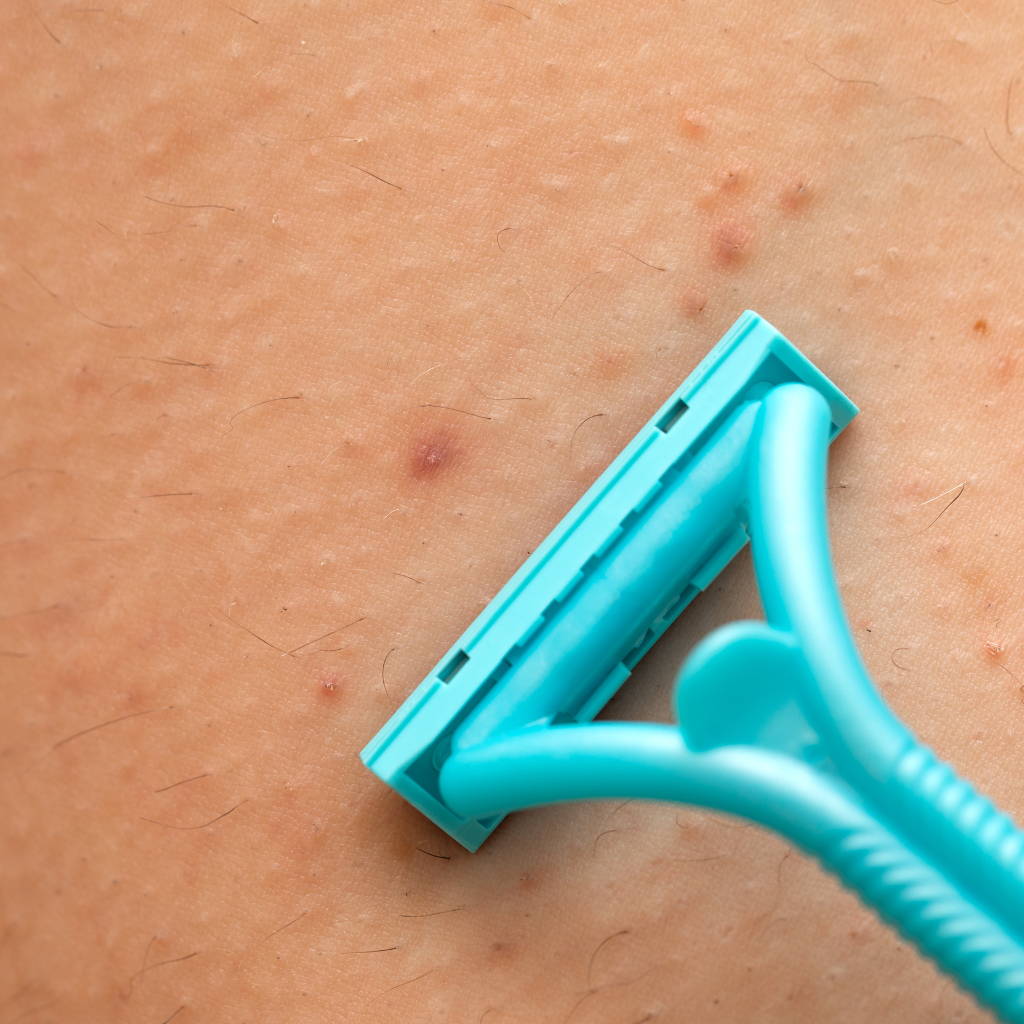
Folliculitis after waxing often shows up as red, itchy bumps a day or two after hair removal. Instead of smooth skin, irritation and small breakouts can appear around the hair follicles, raising concerns about what went wrong.
This guide explains what folliculitis after waxing is, why it happens, how to reduce the risk, and how to manage symptoms safely at home. It also covers when medical care is recommended.
Understanding Folliculitis After Waxing
What Folliculitis Is (And What It Is Not)
Folliculitis is inflammation of the hair follicles, the small openings where hair grows from the skin. After waxing, follicles are temporarily stressed and more exposed, which increases the risk of irritation or infection. It typically appears as small red or white bumps around individual hair follicles and can resemble acne, a rash, or razor burn, though it is medically distinct from all three.
- An inflammatory reaction centered around hair follicles
- Sometimes sterile (just irritation) and sometimes infected (bacteria, yeast, or fungi)
- Often triggered by friction, heat, waxing, shaving, or occlusive products
- Classic acne (though it can look similar)
- An STI or STD (even in the bikini/Brazilian area)
- Always a sign of bad hygiene or a "dirty" salon, though poor hygiene can make it worse
Common Signs And Symptoms After A Wax
Folliculitis after waxing usually appears within a few hours to a few days of your appointment. You might notice:
- Small red bumps centered on hair follicles
- White-tipped pustules that resemble pimples
- Itching, tenderness, or a mild burning sensation
- A rough or “sandpaper-like” skin texture
- Clusters of pus-filled bumps
- Swelling and warmth in the area
- Painful or very tender spots
Who Is More Likely To Get Folliculitis After Waxing
- Have sensitive or reactive skin
- Are acne-prone or have oily skin
- Have curly or coarse hair that is more likely to become ingrown
- Sweat frequently due to activity or climate
- Wear tight or synthetic clothing after waxing
- Have a history of eczema, dermatitis, or keratosis pilaris
- Shave between waxing appointments
Why Folliculitis Happens After Waxing
How Waxing Irritates The Hair Follicle
The Role Of Bacteria, Yeast, And Ingrown Hairs
Once hair is removed, healing follicles are more vulnerable to common skin-related triggers:
- Bacteria:Staphylococcus aureus, a bacteria normally present on the skin, can enter irritated follicles and cause pustules and redness. Poor sanitation practices increase this risk.
- Yeast and fungi: Yeast such as Malassezia can overgrow in warm, moist environments, leading to clusters of small, itchy bumps, particularly on sweat-prone areas.
- Ingrown hairs: As hair regrows, curly or coarse strands may curl back into the skin instead of exiting the follicle, triggering inflammation as the body reacts to the trapped hair.
Post-Wax Factors That Increase Risk
Certain conditions after waxing can significantly raise the likelihood of folliculitis:
- Excess heat or sweating shortly after waxing
- Tight or synthetic clothing that creates friction
- Heavy or pore-clogging products applied to freshly waxed skin
- Inadequate or overly harsh cleansing before or after waxing
Addressing these factors plays a major role in reducing post-wax irritation and recurring folliculitis.
How To Prevent Folliculitis Before, During, And After Waxing
Pre-Wax Prep: Exfoliation, Skin Care, And Hair Length
- Gently exfoliate the area 2–3 times per week using a mild scrub, soft washcloth, or low-strength AHA or BHA.
- Avoid harsh scrubs or sharp particles that can cause micro-tears.
- Cleanse the area well to remove sweat, lotion, deodorant, and body oil. Using a dedicated pre wax cleanser helps reduce surface bacteria without over-drying.
- Make sure hair is the right length, typically about ¼ inch (around a grain of rice). Too short and wax tugs at skin more: too long and removal is more traumatic.
- Skip heavy lotions, self-tanner, and strong actives (like retinoids or strong acids) on the area.
During The Wax: Technique And Hygiene
- No double-dipping in the wax pot
- Clean applicators and linens
- Gloves worn for intimate areas
- Thorough pre-wax cleansing
- Applying wax in the direction of hair growth
- Removing wax parallel to the skin
- Limiting repeat passes
- Monitoring temperature carefully

Post-Wax Care: First 48 Hours And Beyond
- Cleanse gently and soothe the skin.
- A light, non-comedogenic waxing oil can help remove residue and reduce friction.
- Avoid fragranced products, harsh alcohols, and strong actives.
- Hot tubs, saunas, long hot showers, and steam rooms
- Heavy sweating from intense workouts
- Tight clothing and synthetic fabrics over the waxed area
- Tanning beds and direct sun exposure
- Begin gentle exfoliation 2–3 times per week to reduce ingrown hairs.
- Use a calming after-wax or recovery serum to support the skin barrier without clogging pores.
Safe At-Home Treatment For Folliculitis After Waxing
Immediate Steps When Bumps First Appear
Early care can prevent symptoms from worsening:
- Pause waxing or shaving until the area calms.
- Cleanse twice daily with a mild, fragrance-free cleanser.
- Apply a cool compress for 5–10 minutes to reduce heat and itching.
- Wear loose, breathable clothing.
Soothing Remedies And Over-The-Counter Treatments
For more noticeable irritation:
- Use a calming after-wax serum with barrier-supporting ingredients such as panthenol, allantoin, or colloidal oatmeal.
- A short course of 1% hydrocortisone cream may help reduce redness and itching when used sparingly.
- For mild superficial folliculitis on non-intimate body areas (such as the back or chest), a brief course of a benzoyl peroxide wash (2.5–5%) may help. Rinse thoroughly and moisturize afterward.
What To Avoid During A Flare
Certain habits can prolong or worsen folliculitis:
- Picking or scratching bumps, which increases infection and scarring risk
- Aggressive exfoliation while skin is inflamed
- Heavy, occlusive products that trap heat and sweat
- Waxing over active folliculitis
Special Considerations For Different Areas And Skin Types
Bikini And Brazilian Waxing
Folliculitis is more common after bikini and Brazilian waxing due to coarse or curly hair, moisture, and friction from clothing.
To reduce risk in this area:
- Maintain consistent waxing intervals instead of alternating with shaving.
- Cleanse with a pre-wax cleanser and avoid perfumed wipes or harsh soaps.
- Wear loose, breathable cotton underwear and clothing for 24–48 hours post-wax.
- Begin gentle exfoliation a few days after waxing and continue 2–3 times per week.
Face, Underarms, And Other Sensitive Areas
Face (brows, upper lip, chin): Facial skin is thinner and often exposed to active skincare ingredients, which increases sensitivity after waxing.
Risk reduction strategies include:
- Discontinuing topical retinoids and strong acids 7–10 days before and after waxing, as directed by a dermatologist.
- Using very gentle, non-foaming cleansers and avoiding stripping toners.
- Delaying makeup application for several hours, ideally up to 24 hours.
- Avoid strong antiperspirants for 24 hours post-wax; use a gentle deodorant if needed.
- Skip intense workouts immediately after waxing.
- Keep the area clean and dry, using lightweight calming serums rather than heavy creams.
Acne-Prone, Sensitive, And Darker Skin Tones
Certain skin types need extra caution because the consequences of folliculitis can be more long-lasting.
Acne-prone skin:
- Use simple, non-comedogenic products before and after waxing.
- Low-dose salicylic acid may be used between waxes on non-intimate body areas if tolerated.
- Patch-test new products before use.
- Stick to fragrance-free, alcohol-free routines.
- Prioritize barrier support with gentle hydrating serums.
- Inflammation is more likely to result in post-inflammatory hyperpigmentation.
- Avoid picking or squeezing bumps to reduce scarring risk.
- Ingredients such as niacinamide or azelaic acid may help fade dark marks when used away from waxing days under dermatologic guidance.
When To See A Doctor And Medical Treatment Options
Warning Signs That Need Professional Evaluation
Most mild cases of folliculitis after waxing improve with proper at-home care. Medical evaluation is recommended if any of the following occur:
- Bumps spread rapidly or form large, painful clusters
- The area becomes very warm, throbbing, or increasingly tender
- Yellow crusting, oozing, or thick pus develops
- Fever or general illness accompanies skin symptoms
- Redness spreads beyond the waxed area or forms streaks
- Folliculitis repeatedly returns in the same area despite good aftercare

Prescription Treatments Your Dermatologist May Recommend
If a dermatologist confirms folliculitis, they'll tailor treatment to the suspected cause and severity.
Common options include:
- Topical antibiotics (like mupirocin or clindamycin) for bacterial folliculitis
- Oral antibiotics for more widespread, deep, or stubborn infections
- Topical or oral antifungals for yeast- or fungus-related folliculitis
- Topical anti-inflammatory agents to calm the skin
- Short courses of oral anti-inflammatory medication in more severe cases
- Recommend targeted antibacterial or antifungal washes for limited weekly use
- Review skincare and aftercare routines for potential irritants or pore-clogging products
- Help establish a long-term hair removal plan suited to the skin’s tolerance
Take Control Of Post-Wax Skin Health
Folliculitis after waxing is common but manageable. Proper skin prep, clean waxing practices, and consistent aftercare with a pre-wax cleanser, light waxing oil, and calming after-wax serum can greatly reduce post-wax bumps.
Early, gentle care often resolves mild irritation within days. If symptoms persist or worsen, medical guidance helps prevent scarring or ongoing skin issues.
Healthy post-wax skin comes from supporting the skin before, during, and after every wax.

Frequently Asked Questions
What is folliculitis after waxing and why does it happen?
Folliculitis after waxing is inflammation of the hair follicles that appears as red or white bumps, sometimes with itching or tenderness. Waxing temporarily stresses and opens follicles, making them more vulnerable to irritation, bacteria, yeast, or ingrown hairs, especially when combined with heat, sweat, friction, or harsh products.
How long does folliculitis after waxing usually last?
Mild cases often improve within 3–7 days with gentle care. More inflamed or infected cases may last one to two weeks or longer and can require targeted treatment, especially if bumps are painful or spreading.
How can folliculitis be prevented in sensitive areas like the bikini line?
Prevention includes gentle exfoliation a few days before waxing, cleansing with a pre-wax cleanser, and avoiding tight clothing, sweating, and fragranced products for 24–48 hours afterward. Gentle exfoliation and a lightweight after-wax serum can help once the skin settles.
What is the best way to treat folliculitis after waxing at home?
Pause waxing or shaving, cleanse twice daily with a mild fragrance-free wash, and wear loose clothing. Cool compresses, calming after-wax or recovery serums, and short-term 1% hydrocortisone may help. Benzoyl peroxide washes may be used briefly on non-intimate body areas only.
Is folliculitis after waxing contagious or a sexually transmitted infection?
No. Folliculitis is not an STI or STD. While bacteria can sometimes spread to nearby skin, it is not sexually transmitted. Proper hygiene and avoiding picking help reduce spread.
When should a dermatologist be consulted?
Medical care is recommended if bumps spread rapidly, become very painful, ooze pus, cause fever, recur frequently, or leave dark marks or scars, particularly on the face or bikini area.